The Local newsletter is your free, daily guide to life in Colorado. For locals, by locals. Sign up today!
What is Pain?
A look at the physiology and psychology behind why we hurt.
When it comes to evolutionary advantages, pain ranks right up there with the opposable thumb—the one you occasionally smash with a hammer. That’s because pain is essentially the body’s way of telling the brain, “Hey idiot, something is wrong. Fix it!” (Technically speaking, it’s the result of a series of signals sent along your neural networks to your brain, which determines what to do with the info.)
But that’s just the physiological explanation. There’s an emotional component to pain, too; a matter of perception that makes what should be an objective stimulus (hammer, meet thumb) a subjective experience (“Ouch!). “There is a complex interplay between the body and the mind,” says Dr. Michael McCeney, a Kaiser Permanente pain medicine specialist based in Lafayette. “Some people have a different threshold for what causes a painful response. But we don’t really understand why.”

So that is the $560 billion question—the estimated amount chronic pain costs the United States every year, according to a 2011 report by the Institute of Medicine (the most recent figure available). The report itself is the result of a clause in the 2010 Patient Protection and Affordable Care Act that required the Department of Health and Human Services and the Institute of Medicine to “increase the recognition of pain as a significant public health problem in the United States.” Roughly 100 million Americans endure chronic pain, to say nothing of the many millions who suffer acute pain from, say, wiping out on that double black diamond run or eating pavement on the way down Lookout Mountain.

Coloradans’ penchants for such activities—and, relatedly, accidents—might help explain why the state is also a hub for pain research. Take University of Colorado Boulder professor of psychology and neuroscience Tor Wager. Using brain-imaging techniques, Wager and researchers at other universities have identified a distinct neurologic signature for pain that’s the same across different people. That’s a step toward being able to objectively measure pain. What’s particularly interesting is that the signature isn’t confined to the part of your noggin that carries pain information—it’s in several brain networks, including areas associated with emotional response. “Now we have evidence that [with pain] there are multiple things going on in the brain,” Wager says.
A greater understanding of what pain is has helped usher in multimodal approaches to treatment, such as those being used at the Center for Integrative Medicine at University of Colorado Hospital. And this January, Kaiser Permanente opened an Integrative Pain Service at its Lafayette Rock Creek Medical Offices, where physicians, pharmacists, physical therapists, and psychotherapists tackle pain together. “One of the most promising areas of pain medicine is turning around the way patients think about their pain,” McCeney says. “One of the most successful treatment options is to help them better accept the fact that they’re in pain and learn how to live with it.” —KC
Rank your own agony index at 5280.com/ouch.
—Images courtesy of iStock
Hard Target
A CU professor finds a non-addictive way to treat pain.

When your brain registers pain, but there’s no physical reason for it, it’s called pathologic pain, and for tens of millions of Americans, it’s a difficult-to-treat chronic condition. But Linda Watkins, a professor of psychology and neuroscience at the University of Colorado Boulder, appears to have discovered a treatment that just might bring relief.
Traditionally, physicians have used opiates such as morphine to treat pathologic pain, but morphine is highly addictive, riddled with lousy side effects, and can be ineffective. Opiates target neurons; Watkins’ treatment focuses on nonneuronal glial cells instead. Glial cells surround neurons, and while they’re not able to transmit the “pain” message to your brain, they’re the ones yelling, “Do it!” to encourage the neuron to deliver the information. With pathologic pain, glia simply don’t shut up, so the neurons keep transmitting false pain alerts. Watkins and her team have been working on a way to silence glia in those situations.
Their solution: XT-101, a nonviral gene therapy. When injected into cerebral spinal fluid or a painful joint, XT-101 encourages the body’s production of Interleukin-10, an anti-inflammatory protein produced naturally that calms glial cells down. Working with Lafayette veterinarian Robert Landry, Watkins has shown through research that a single injection of XT-101 can reduce chronic pain for three months in dogs suffering from arthritis and joint issues. “It really gives me hope that it’s going to transfer to people,” Watkins says. What’s more, the injection isn’t a narcotic, so it doesn’t appear to have the same kind of addiction potential as morphine.
XT-101 is currently awaiting approval by the FDA for investigational new drug status; Watkins expects that to happen this year, meaning she could begin testing on humans as soon as she raises the millions she needs. Meanwhile, the results of another, similar drug she helped develop, Naltrexone, are so encouraging that the Department of Defense has funded research to test Naltrexone’s ability to reduce chronic pain and drug abuse in soldiers and veterans. —Daliah Singer

—Images courtesy of Linda Watkins; Sean Parsons (icons)
Hurts So Good
Many of Coloradans’ favorite pastimes require a little misery, too. What makes us able to tolerate the pain in pursuit of pleasure?

Mental toughness. Tenacity. Determination. Call it what you like, these buzzwords are often used by sports commentators to describe pain—specifically, an individual’s ability to overcome it. Some of us are just better at that than others: cyclist Tejay van Garderen, climber Tommy Caldwell, runner Shalane Flanagan, and almost every hockey and football player we’ve met come to mind. But why?
“That’s part of the holy grail of pain medicine,” says Dr. Michael McCeney, a Kaiser Permanente Colorado pain medicine specialist and competitive cyclist. “We don’t fully understand, but it has to do with how people perceive pain and whether they’re in control of it.” He explains: Athletes and weekend warriors who are able to interpret their pain in a positive way—as part of the pursuit of a goal like winning the race—endure the leg- and lung-searing better than the rest of us, who regard the discomfort as a negative. The good news (especially here in the country’s fittest state, where skiing, cycling, running, climbing, and paddling are as much a part of our collective culture as beer and the Broncos) is that you can get better at it.
The first step is “developing the ability to see your thoughts,” says Dr. Christa Smith, a clinical psychologist who specializes in mindfulness and cognitive behavioral therapy (CBT) as a way to manage pain. Doing so frees you up to interpret those thoughts differently. Instead of perceiving your quaking quads as a bad thing as you hoof it up the Manitou Incline, consider the positive aspects of what that pain means: that your legs are going to look great in those new shorts, or that you’re getting closer to a spectacular view or closer to a piece of pecan pie from Front Range Barbecue once you’re down.
That’s the cognitive part. The behavioral part is actually finishing the task. Then there’s receiving your reward, whether that’s the view, the pie, or just being done. Psychologists call this the reinforcing moment. (Pavlov called it dinner.) “Some people have a connection with that reinforcing moment earlier than others,” Smith says. That might explain why they’re better at setting aside their physical anguish; they’re just more practiced. You can be, too. Many meditation and fitness centers offer mindfulness classes, or you can work with a private practitioner like Smith.
Or, you can simply get a bit older. That’s part of what ski mountaineer Hilaree O’Neill, the first woman to climb two 8,000-meter peaks (Everest and Lhotse) in 24 hours, attributes her success to. Says the 42-year-old Telluride resident: “Once you’re 35 to 50, you just get better at suffering.” —KC
Colorado Broke My _____!
Dr. Jarrod King, director of Denver Health’s sports medicine team, and Dr. Eric McCarty, chief of sports medicine at the University of Colorado School of Medicine, break down common injuries from some of our favorite activities.

For the Love of the Game
In the 12 years Broncos inside linebacker and Pro Bowler Karl Mecklenburg spent in the NFL (’83 to ’94), he missed only five games. Still, in many of the 180 contests the Broncos Ring of Famer lined up for, he was hurt. Now 54, Mecklenburg has undergone 17 football-related surgeries. And that’s just counting stuff they could fix with a scalpel. “There is a weeding-out process in football,” says the Littleton resident and motivational speaker. “If you don’t have a high pain tolerance, you don’t enjoy the game. If you don’t enjoy the game, you don’t do well and quit—or are fired.” Here, a look at what it takes to make it in the NFL. —KC
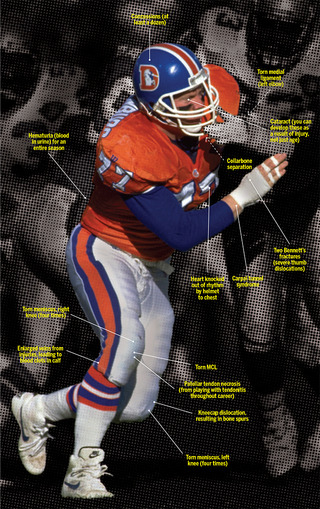
—Images courtesy of Shutterstock; Sean Parsons (icons); Eric Lars Bakke/Denver Broncos
The Replacements
Why trading out knees, hips, and shoulders doesn’t always mean trading up.

Here in the land of mountains and rivers and big skies, it’s tough to say no to skiing, cycling, kayaking, and everything else. So what if our love of an active lifestyle is slowly breaking down our body parts? With improvements in replacement knees, shoulders, and hips, we can just get new ones. Right? “Well, that’s kind of terrifying from a surgeon’s perspective,” says Dr. Jarrod King, a Denver Health arthroscopic surgeon and director of the sports medicine team. “What you have in your body is a living biological system that was designed to last your whole life. Even with improvements, none of these replacements are going to be as good as the parts they’re replacing.”
OK. So there’s that.
The reality is, though, that docs are replacing hips, knees, and shoulders in younger patients than they were 20 years ago—patients are often in their 50s and, in some cases, their 40s. While upgrades in materials have improved the durability and functionality of replacements, they’re still not designed to last more than 12 to 20 years (eight to 10 for shoulders). Which means going under the knife a second time remains a likely possibility, especially if you drive your new part the same way you did the original.
A second surgery can be more daunting than the first for reasons beyond the standard risks of infection, particularly when we’re talking about shoulders. “Anytime you have to take the metal component out, you have to take out additional bone,” King explains. “The shoulder has very little bone to work with. So you’re at a very high risk of running out of wall to hang your picture on.”
Forty-four himself and an ardent mountain biker and skier, King understands the desire to savor Colorado’s outdoor playground. He doesn’t suggest giving any of that up. Just maybe consider shelving those 20-foot drops. “I love to do all the stuff that makes Colorado tick, too,” he says. “I’ve just backed off a little, so I can do it longer.” —KC
Muscling Through
Meet Greg Roskopf, the Englewood man behind #18’s extended career.

Broncos fans can thank a rock quarry in Iowa for extending Peyton Manning’s career. That quarry is where, in 1982, William Penn University linebacker Greg Roskopf fell 20 feet, suffering a lower lumber compression fracture. Eighteen years later, the injury would lead Roskopf, now a sports medicine specialist, to develop Muscle Activation Technique (MAT), a treatment for musculoskeletal imbalance that Manning has been receiving once a week for the past six years. (He flew Englewood-based Roskopf to Indianapolis every two weeks before Denver snagged the QB in 2012.) In a 2012 Sports Illustrated piece, Manning credited MAT for helping prolong his career. Fortunately for you and me, the treatment is not just for the pros.
Muscle Activation Technique is essentially a highly personalized assessment and treatment of imbalances in body mechanics that Roskopf developed over the course of about 10 years, largely in search of his own relief. Despite taking a year off from football in college, Roskopf’s back continued to plague him into his 20s. While completing his master’s in physical education, he also started experiencing knee and foot problems. “I thought, If I’m this bad at 25, what am I going to be like at 50?” So between his jobs as a strength and conditioning coach for California State University Fresno and later the Utah Jazz, he studied the interconnection of the musculoskeletal system, attending seminars with the foremost specialists in everything from sports medicine to podiatry. In 2000, he put it all together in MAT.
Here’s how it works: When the body senses instability, as with an imbalance or injury, Roskopf says, the brain sends a message to tighten the muscles in that area. Over time, this constant contracting can lead to inflammation and biochemical changes that can alter communication between the brain and muscles. Roskopf likens it to a loose car-battery cable. Your brain sends a message to the muscles to contract, but they don’t always receive it. So other parts of your body compensate, and the cycle of imbalance continues. MAT seeks to end the cycle by stimulating those nonfiring muscle fibers.
“Hop up here,” Roskopf says, patting an examination table inside his Englewood office. “I’ll show you.” I crawl up on the table and lie on my back. Roskopf takes me through the same series of foot and leg positions he would any new patient. Within no time, he’s discovered a hip imbalance on my right side: When he holds my leg at about two o’clock and asks me to push up against his hand, I can’t. Try as I might, my leg won’t resist the pressure—Roskopf easily presses it down with his index finger. It’s maddening—and surprising. Like many Coloradans, I’m a fairly active and fit person, and one of the lucky ones without severe chronic pain. That I can’t make my leg perform a simple movement comes as a (frustrating) shock.
Roskopf isn’t surprised. “Most people have some kind of imbalance,” he says. “You might not feel it now, but if you’re not getting proper alignment, you’re an injury waiting to happen.” Correcting the imbalance requires stimulating my nonresponsive muscles— something Roskopf does by gently palpating the length of each of the involved muscles, including where they connect to joints. We go through the series of tests again, and I pass. I can resist his hand, no problem.
Manning’s treatment is a little more involved; it also includes specific exercises that test imbalances under stress and work to strengthen them. MAT has proved effective enough that Roskopf has been contracted to treat the whole Broncos team. And the Nuggets. And Carson Palmer, Terrell Davis, and injured swimmer Amy Van Dyken. Oh yeah, and the athletes at the NFL combine. It’s also why Roskopf has a six-month-long waiting list for new patients. Fortunately, there are about 100 other practitioners in Colorado, including several at the MAT corporate headquarters in Englewood—that’s who Roskopf sees twice a week. Now 51, Roskopf has a very different response to that question he asked himself all those years ago—What am I going to be like at 50? The answer: pain-free and functional. And in the case of (younger) athletes like number 18, that also means being able to perform at a high level for longer. Hopefully long enough to bring home the Lombardi trophy. —KC
—Images courtesy of Sean Parsons; Matt Nager
The Pain Of Doing Nothing
Sitting in front of a computer all week can be a real pain in the neck (and back and legs). That’s why we asked Nick McElhiney, an Erie ergonomist, to pick three devices to help correct our cubicle sins.
 Hammy-Strung
Hammy-Strung
Sitting with hips, knees, and elbows all at right angles winds tendons and hamstrings tighter than a tax accountant come this time of year. Hag, from ergonomics-obsessed Norway, designs tall chairs with multiple heights and seating positions that keep your hips above your knees and force your legs into an active position (unless, of course, you want to fall over). From $568, haginc.com
 The Agony Of The Feet
The Agony Of The Feet
Being seated all day is exhausting. That’s because when the body is static, the heart and lungs have a hard time fueling muscles. And standing desks open another can of sedentary worms, such as blood pooling in the feet and varicose veins. The best option: The motorized GeekDesk moves between sitting and standing mode to keep you up (and down) and moving. From $749, geekdesk.com
 Type Oww
Type Oww
One size fits all often means one size fits none, and that’s true of keyboards, too. Most workers must angle their wrists awkwardly to position their hands properly—a move that can put them at risk for carpal tunnel. Goldtouch’s adjustable keyboard splits open and rotates out, keeping wrists at comfy angles so your days of typing don’t end up spelling m–i-s-e-r-y. From $105, goldtouch.com —Spencer Campbell
Get Back To Where You Belong
Denver physical medicine and rehab specialist Yani Zinis reveals what 18 years of treating back pain have taught him.
If you’re a living, breathing adult, chances are you’ve suffered back pain: It afflicts 80 percent of the population and is the second most common cause of emergency room visits. With sufferers spending more than $17 billion a year in search of relief, back pain ranks as one of the country’s 15 most expensive medical conditions, according to the Institute of Medicine. But how do you know when a tweaked back is a passing hindrance or something more serious? Dr. Yani Zinis, a longtime team doctor for the Colorado Avalanche who also practices at Denver’s Orthopedic Associates, outlines what he’s learned about diagnosing, treating, and living with back pain in 18 years as a specialist. —Luc Hatlestad

—Images courtesy of Izzyplus; Geekdesk; Goldtouch; Bryan Grant
The Five-Year Ache
For five long years, Lafayette resident Rebecca Benson lived with a debilitating headache night and day—until a Front Range doctor used a technological innovation to finally put a stop to the pain.
Rebecca Benson can still remember the day it started. In 2007, the then-39-year-old Lafayette resident came home from her job as a receptionist for a law firm with a painful headache. “It was a stressful day,” she remembers. “I figured I’d just sleep it off.”
When she woke the next day, though, the pain was worse. Debilitating. Tylenol didn’t work, and she was allergic to Advil. She went to work but left in agony by midafternoon. When the pain wasn’t gone a week later, she visited her primary-care physician. That doc became the first of 26 physicians Benson would see over the next five years—years marked by an excruciating headache that never relented. Every day, every hour, the torment continued.
She left her job. (The pain prevented her from staying long enough to get her work done.) She missed out on her daughter’s high school activities. (“Apparently I went to some of her softball games,” Benson says, “but I don’t remember being there.”) She couldn’t take vacations. (Over five years, Benson left the state only once.) But the worst part, Benson says, was that no one could tell her what was wrong with her. Dozens of brain scans ruled out an aneurysm or dangerous tumors, but at least 50 different medications all failed to subdue the pain. “It’s very disheartening when you go through that many doctors and no one can tell you that someday you’re not going to have a headache, that you’ll be able to enjoy life again,” she says.

In 2009, Benson began seeing Dr. Michael McCeney, a Kaiser Permanente Colorado pain medicine specialist. He was number 26. At the time, Benson had a diagnosis of carotidynia, a pain syndrome that comes from the carotid artery in the neck. McCeney added occipital neuralgia (irritation of the occipital nerves that causes pain or tingling) and atypical facial pain. For three years, McCeney tried everything: injections in her neck, Botox shots in the back of her head, surgery to remove a small, benign mass in her neck. Some things helped a little, but only for a short time, and they’d eventually lose their effectiveness altogether. “She was on some pretty high doses of pain medication,” McCeney says. “And it was barely keeping her afloat.” In 2012, McCeney suggested they move on to what is considered the most aggressive treatment for nerve pain: spinal cord stimulator technology.
Most commonly used to treat pain related to the spine, a spinal cord stimulator is typically implanted just beneath the skin near the back of the hip. Wires run under the skin, delivering electrical pulses to the spinal cord itself, which—though no one knows for certain—is thought to block the pain signals going to the brain. In Benson’s case, though, the wires would run all the way up to the occipital nerves on either side of the base of her head. These nerves synapse with nerves near the headache center of the brain. This technology has been around since the 1970s, but recently, as the technology has become more sophisticated, it’s become more common. (McCeney and another Kaiser Permanente Colorado doctor perform about five to 10 stimulator implant surgeries a month.) Popular Mechanics even recognized the technology in its 2014 Breakthrough Awards. “Still, we consider it a treatment of last resort because it requires surgery, and you’re implanting a foreign object in the body,” McCeney says. Potential risks include complications from surgery, infection, and the wires moving under the skin, thus rendering the device useless.
Benson didn’t care, not even that it might require two surgeries: one to implant temporary stimulator wires to see if it relieved her suffering and a second to implant a permanent device. (And subsequent surgeries would be needed to replace the “permanent” device, which has a life of five to 10 years.) As soon as she woke up from the first procedure and they turned the stimulator on, Benson turned to McCeney and said, “Schedule the next surgery.” The pain was finally gone. That was three years ago, and Benson has been pretty much headache-free ever since. She’s also o_ all her narcotic pain medications. McCeney went from seeing Benson every few months to only twice in the past three years for minor adjustments. “He’s on my list of miracle workers,” Benson says. “Life is back to normal. I can do everything I could before. We’re able to travel without worrying about a doctor appointment or if I’ll get sick. I’ve been back East to see family and gone on two Caribbean cruises. I can just pick up and go whenever. In fact, I think I’m about ready to go back to the beach now.” —KC
Head Case
Local docs and researchers offer new answers for the age-old problem of migraines.

More than 30 million people in the United States suffer from migraines, at a cost to the U.S. economy of a headache-inducing $14.5 billion per year. I’m one of them. If you haven’t ever had a migraine, I know what you’re thinking: It’s a headache. Take some Advil. Get over it. To which I would respond: Grab an ice pick. Shove it through your eye and into the back of your brain. Now, let me know how that’s working out for you. Migraines are not typical headaches; for me, the pain is so severe that even laying my head on a pillow is excruciating. Women, who are three times more likely as men to suffer from migraines, have been known to compare the pain to childbirth—and not unlike the process of bringing a child into the world, the pain of a migraine can last anywhere from four to 72 hours.
Fortunately, doctors and researchers in Denver have moved beyond the take-two-of-these-and-call-me-in-the-morning approach to treatment. Dr. Emily Bates, an assistant professor at the University of Colorado School of Medicine, is studying the effect of estrogen on the etiology of the headaches. And doctors at the two-year-old University of Colorado Hospital headache clinic are using more integrative approaches to provide relief. There, headache specialists discuss lifestyle changes with patients (sleep, diet, exercise, weight, depression, anxiety) and tailor-make cocktails of different drugs—among them, antidepressants and anti-seizure and blood pressure–lowering meds—for each patient, continually tweaking prescriptions to make them as effective as possible. Such personalized care provides hope that those who have, until now, been beyond the reach of most common migraine treatments won’t have to “get over” anything much longer. —Geoff Van Dyke
—Image courtesy of University of Colorado Hospital








